Psoriasis is not a direct threat to the life span, but the quality. Any stage or form of the disease, the patient wears the stigma “leper” taken out of the world.
Healthy people are shying away from contact with a patient with psoriasis – in time, this has a very strong impact on his life social, professional and emotional, in some cases even leading to suicide (5% of those affected).
Psoriasis is not a contagious disease
What is < psoriasis > A chronic skin condition, very common (immediately after pruritus but more debilitating than this), as serious as diabetes, high blood pressure or depression. Past research has established that the disease is genetically determined – most likely on his mother – and the same genes considered responsible for the development of diabetes and obesity.
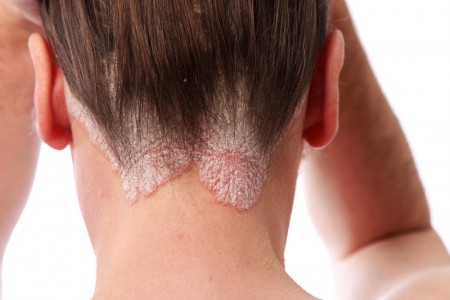
< Symptoms > is manifested by the appearance of reddish spots and round, with well defined edges and covered by skin peels overlay color whitish to silver. In some cases, these areas produce itching.
At the onset, cutaneous eruption can be discreet and limited: only a red plate located at the joints most requested (elbows, knees) or scalp hair in hidden areas. Very quickly, redness turn into large spots covered by silvery scales in the shape of scales. Besides traumatising appearance these hinder and limit the movements of the patient, up to immobilize him.
< Who > It is more common in whites and very low in people of color or Asian. Men and women are affected equally, but can occur earlier in women.
< Age > Can occur at any age, even in the first months of life, but usually occurs between the second and third decade of life. The statistics indicate the age of 28 years as the most common for triggering the first episode.
< Duration > It is a chronic disease and can take several years, sometimes entire life, with periods of remission and relapse. Its evolution is different from one person to another, flares being the most difficult to bear. Only a very small proportion of patients suffering from psoriasis with continuous evolution and on mostly of the body.
< Causes > At the base of disease stand genetic alteration, hereditarytransmitted and influenced by environmental factors. The causes of this disease are not entirely known. Recently a group of researchers from the University of Rome has succeeded in demonstrating the genetic origin of the disease and identify the “failure” of several genes responsible for cell activity keratocite, located in the outer layer of the epidermis.
It is assumed that genes that cause disease are applied and activated by infections caused by a virus of the herpes family. These infections lead to immune imbalance in the body is no longer able to control the disease.
Triggering factors
-Emotional stress or psychological events strong
-Physical injuries (burns, surgical scars, bruises low intensity random but frequent the same place)
-Medications (lithium, beta-blockers). Some forms of steroids may lead to worsening disease when dosage reduction or suspension.
-Beta-hemolytic streptococcal infections (tonsillitis)
-Eating calcium-free
-Hormonal imbalance – occurs at puberty, menopause.
-Alcoholism and smoking
 < Treatment >
< Treatment >
There is no cure for psoriasis, only an intervention at the genetic level could lead to his disappearance. But there are effective treatments for shortening flares and determining remission.
There are cases in which psoriasis heal itself, but they are rare and only very mild types. The effect of drugs is conditioned individual response, so treatment must be strictly controlled to avoid medical complications, generalization and the unfavorable lesions.
Treatment strategy varies greatly depending on the extent and location of disease. Being a chronic disease requiring prolonged treatment psoriasis. Therefore, medication used must be safe in long-term administration and devoid of side effects.
Allopathic treatment includes an attack phase, in which remove skin lesions and one maintenance. It may be topical (external and local) for mild forms often accompanied by the systemic (internal medicine), in severe forms.
 < Phototherapy >
< Phototherapy >
Very employed in recent times, it is based on application of ultraviolet type A and B (UVB low intensity) with fluorescent or halogen.
Thermal cure has a beneficial effect on skin regeneration, relieving itching. Due to their properties, thermal waters have a decongestant and antiseptic action, contributing to disease remission. Dead Sea (Israel) is an ideal place to treat psoriasis, but a heliotherapy Black Sea has similar effects.
How is the life of a patient with psoriasis
Psoriasis is considered by outsiders, a contagious disease or generated by lack of personal hygiene. From here, and the reaction of others that they can not hide the fear and reluctance to those with this disease.
The skin of a patient with psoriasis who is in the acute phase inspire abhorrence and a strong rejection response, even at people who know that the disease is not contagious.
People do not want to shake hands with a patient with psoriasis, mothers will not leave their children in caring of a educator, schoolteacher or teachers with psoriasis, customers can disappear suddenly from the front of desk where a person operates with skin attacked of psoriasis.
Most occupations related to interacting with people can be seriously affected by the occurrence of disease. In addition to career issues, patients have to face public stigma and the emotional.
Severe forms of psoriasis can prevent patients to work, have access to public facilities (swimming pools, health clubs, beaches) or to have sex (especially women). Patients consuming more alcohol and tobacco – risk factors for disease manifestation.
So they enter a vicious circle in which the stress of the disease contributes to its maintenance and worsening . Patients have feelings of guilt and shame are more sensitive to the attitude of others. Ten percent of them had suicidal thoughts, compared with 3% to sufferers of other diseases.
About Psoriasis in figures
Psoriasis affects between 1.5 and 3% of the population of North America and Europe, with higher incidence in Denmark and other Northern European countries and low in Central Asia and Eastern Europe, where the figures are below 0.4%.
According to a study conducted among patients with psoriasis, 52% said they felt embarrassed or ashamed in relationships with others because of their disease and 53% said that the disease affects their leisure activities choices. In order not to be judged by those who come in contact, 40% of patients hide their disease, and 21% give up to befriend new people. The survey also shows that for 23% of respondents, professional life suffered after the diagnosis of psoriasis, while for 34% of relationships with colleagues were changed. Also, 32% have hidden superiors and colleagues as suffering from psoriasis.
If triggering the disease, doctor recommends:
-
Avoid self-administration of medication or the pharmacist’s recommendation. Each patient needs a personalized treatment determined only by specialist (dermatologist).
-
Do not call the “healers” and homemade salves – unfair treatment empirically determine the evolution of aggressive disease harder to treat severe complications that require further systemic therapies with high toxicity and side effects.
-
Avoid dry skin. We recommend a daily massage of the entire body with an emollient, moisturizing, especially after your bath or shower and your skin is drier.
-
Use cotton clothing and avoiding wool and synthetic materials.
-
Avoid, as you can, stressful situations.
-
Powering up easily with more vegetables and fruits and protein light (no fat and concentrated sweets). Keep your weight in the normal range.
-
Do not scratch the lesions. Avoid, if possible, continuous trauma and temperature variations.
-
Quit stimulating substances, smoking and excess alcohol.
[adsense][adsense]